A fundamental component of Cognitive-Behavioral Therapy is the idea that our thoughts, emotions, and behaviors all influence one another. This is important because it suggests that we can change how we feel by changing how we think and what we do. The connection between thoughts and emotions was somewhat explored in my last post, so today I wanted to focus on the connection between what we do and how we feel.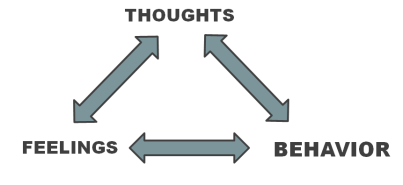
Runners experience a “high” when pushed to their limits, we often feel better after a “good cry”, and we feel pride and satisfaction when we improve at an important task. Conversely, we feel guilty after erupting in anger, we feel sad when we isolate, and we feel anxious when we drink 9 coffees. Therapists typically have an assortment of “relaxation skills” that they teach to their clients to use when they are upset.
When you enter therapy, most therapists will usually assess your sleeping patterns, your diet, your exercise routine, your daily habits, and your hobbies. This is because what you do, greatly impacts how you feel and what you think. Improving self-care can greatly impact a person’s physical and mental health.
 The question of “how do we lead a healthy life” has been explored by humans for a very long time. Researchers at SFU have been attempting to modernize the very old idea of the “Wellness Wheel.” This model breaks down the concept of wellness into seven primary dimensions Simply put, we can improve our wellness by attempting to maintain balance among these dimensions. I suspect most people can anticipate how their well-being would suffer if they were to over focus on one dimension at the cost of the others.(http://www.sfu.ca/students/health/resources/wellness/wheel.html).
The question of “how do we lead a healthy life” has been explored by humans for a very long time. Researchers at SFU have been attempting to modernize the very old idea of the “Wellness Wheel.” This model breaks down the concept of wellness into seven primary dimensions Simply put, we can improve our wellness by attempting to maintain balance among these dimensions. I suspect most people can anticipate how their well-being would suffer if they were to over focus on one dimension at the cost of the others.(http://www.sfu.ca/students/health/resources/wellness/wheel.html).
In my opinion, few examples illustrate the connection between emotions and behavior  better than the behavior habits of depressed people. When you ask a person with depression about their daily routines, it is not unusual in my experience for them to describe a daily routine dominated by social withdrawal, minimal exercise, low goal-oriented behavior, unhealthy eating habits, and irregular sleeping patterns. Paradoxically, depression often reduces self-care which in turn feeds depression. I’ve often believed that if we were to take a mentally “healthy” person and force them to behave the same way as a depressed person, it would only be a matter of time before the despair, sadness, and loneliness set in. Regardless of what came first, research suggests we can reduce feelings of depression by improving self-care.
better than the behavior habits of depressed people. When you ask a person with depression about their daily routines, it is not unusual in my experience for them to describe a daily routine dominated by social withdrawal, minimal exercise, low goal-oriented behavior, unhealthy eating habits, and irregular sleeping patterns. Paradoxically, depression often reduces self-care which in turn feeds depression. I’ve often believed that if we were to take a mentally “healthy” person and force them to behave the same way as a depressed person, it would only be a matter of time before the despair, sadness, and loneliness set in. Regardless of what came first, research suggests we can reduce feelings of depression by improving self-care.
Behavioral Activation (BA) is a strategy for combatting depression that has over 40 years of research supporting it. Eight common techniques used in BA are (1) Activity monitoring, (2) value and goal assessment, (3) activity scheduling, (4) skills training, (5) relaxation skills, (6) contingency management, (7) procedures targeting verbal behavior, and (8) procedures targeting avoidance. BA techniques can help challenge the belief that we are victims to our moods, that we can’t do what is good for us until we feel better. These techniques can demonstrate that sometimes we can “fake it to we make it.” Please see the “Self-Help Resources” page for more information about BA.
This idea that there is a connection between our mood and our behavior can benefit anyone, not just those with clinical depression. The cliché’ and famous Einstein quote is “the definition of insanity is doing the same thing over and over and expecting different results.” By that logic, can we really expect our mood to change when we are unwilling to change what we are doing (or thinking)?
Please feel free to e-mail me with any questions or comments.